 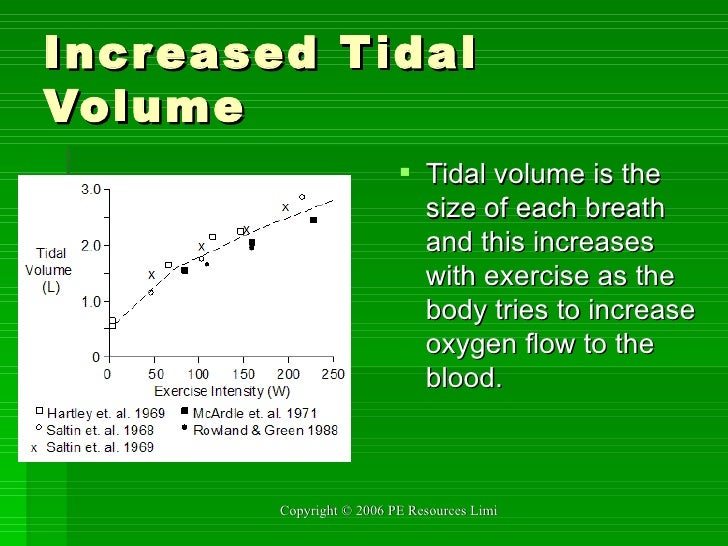 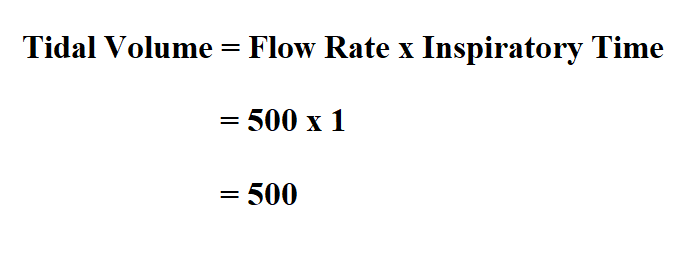
The independent samples t test was conducted to assess for potential difference in overall PIP by group (NIV-NAVA vs. Data were recorded separately for each variable without time stamps and subjects had variable numbers of observations for P-Peak and VT therefore, the P-Peak values and the VT values could not be linked by observation. Based on clinical rationale, each observation is viewed as independent therefore, the statistical analysis was conducted on the full set of observations. We therefore planned to evaluate the range of PIP and VT that premature neonates generate while on NAVA.Įxamination of data included calculation of summary statistics for continuous data, along with frequencies and percentages for categorical data. Despite NAVA’s neuro-ventilatory coupling advantage that NAVA ventilation provides, concern has been raised that enabling premature neonates to choose their own ventilator parameters could result in excessively high PIPs and VTs, theoretically increasing the risk of pneumothorax acutely, and chronic lung disease over the long term. By optimally supporting native breathing reflexes, NAVA can facilitate patient effort in a synchronous fashion. Studies have shown that neonates, while in both invasive and non-invasive NAVA, have the ability to “switch-off” neural inspiration, and then cycle-off the ventilator when an appropriate volume/pressure has been reached. When properly positioned, it can accurately and reliably trigger and cycle the ventilator breath, independent of airway leaks, making it ideal for synchronizing non-invasive ventilation. This Edi signal is obtained from a specialized indwelling nasogastric feeding tube with embedded sensing electrodes (NAVA catheter). The patient controls the amount of pressure delivered by the ventilator using the electrical activity of the diaphragm (Edi) waveform to trigger-on and cycle-off each assisted breath, therefore providing truly synchronized ventilation. Neurally adjusted ventilatory assist (NAVA) ventilation allows patients to control their own peak inspiratory pressure (PIP) and VT on a breath-to-breath basis. Typical VT ranges to initiate tidal volume ventilation (VTV) range from 4 to 7 ml/kg. Data for selecting the appropriate target tidal volume (VT) for specific patients with different clinical conditions are limited. When compared to pressure-limited ventilation, the use of volume-targeted ventilation has been associated with more favorable outcomes. Despite advancements in neonatal ventilation modalities, premature neonates remain at significant risk for bronchopulmonary dysplasia (BPD). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
